A new analysis of data from the 2013-2014 Zika epidemic in French Polynesia by scientists from the Institut Pasteur, Paris, and their French Polynesian colleagues has confirmed the incidence of grouped cases of microcephaly and quantified the risk of microcephaly associated with the virus. Using innovative mathematical modeling techniques, their research shows that the risk of microcephaly is around 1% for a fetus or newborn whose mother has been infected by the Zika virus during the first trimester of pregnancy. Their findings have been published in the journal The Lancet.
© Institut Pasteur
An epidemic caused by Zika virus disease is currently affecting several countries in the Americas. The emergence of this epidemic has coincided with a dramatic increase in the number of suspected cases of microcephaly, a severe neurological defect characterized by fetuses and newborns with unusually small heads. The data from this ongoing epidemic has yet to be consolidated and is hard to interpret, especially when it comes to quantifying the risk of microcephaly associated with Zika infection.
This led scientists from the Institut Pasteur – in the Mathematical Modeling of Infectious Diseases Unit, led by Dr. Simon Cauchemez, and the Epidemiology of Emerging Diseases Unit, led by Prof. Arnaud Fontanet – in collaboration with Henri-Pierre Mallet from the Public Health Surveillance Office in French Polynesia, Marianne Besnard from the French Polynesia Hospital Center, and the Necker and Trousseau Hospitals in the Paris Public Hospital Network (AP-HP), to focus their research on data from a previous Zika epidemic in French Polynesia. Their retrospective study identified all the cases of microcephaly that occurred over a period of 23 months between September 2013 and July 2015.
Their analysis initially revealed that, of the 8 cases of microcephaly identified, 7 (88%) occurred during the 4 months immediately following the Zika epidemic, suggesting a strong temporal link between the epidemic and the incidence of microcephaly.
To help them characterize this link further, the scientists then developed mathematical models to determine the period of pregnancy during which infection with the Zika virus was most likely to be associated with an increased risk of microcephaly. Their model showed that 1% of fetuses or newborns whose mother was infected during her first trimester of pregnancy had microcephaly, compared with a normal risk of 0.02%.
This level of risk per infected pregnant woman is lower than the risk observed for other viral infections associated with complications during pregnancy. For pregnant women infected by rubella during the first trimester of pregnancy, for example, the risk of severe complications is estimated to be between 38% and 100%. These results remain a cause for concern, however, since unlike rubella, which affects fewer than 10 pregnant women each year in France, the proportion of people infected during a Zika epidemic can exceed 50%. These findings confirm the need to protect pregnant women from the virus, especially during the first trimester of pregnancy.
This study follows on from other research that has revealed the presence of the Zika virus in the amniotic fluid or brains of fetuses medically aborted after being found to have microcephaly, and a study showing that neural stem cells can be infected by the Zika virus. Further research is now needed, especially involving prospective cohorts of pregnant women, to identify all the congenital anomalies that may occur at different periods of pregnancy following infection by the Zika virus, and to determine whether the presence of clinical signs in mothers infected by the Zika virus increases the risk of microcephaly.
This research was co-funded by the aforementioned institutions and by the LabEx IBEID, EU-PREDEMICS, NIH-MIDAS and the AXA Research Fund.
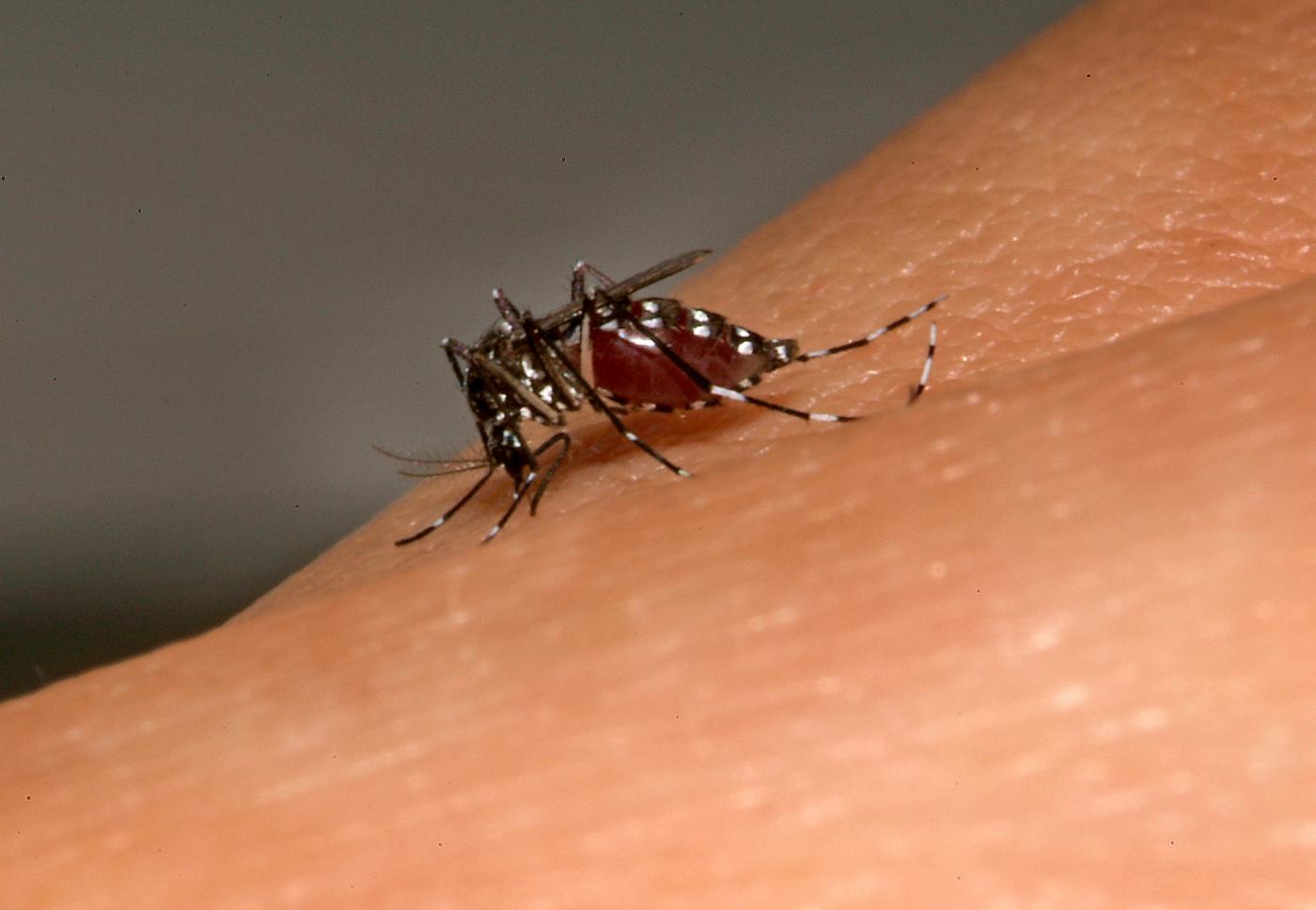
To learn more, read the Zika fact sheet.
Source
Association between Zika virus and microcephaly in French Polynesia, 2013-2015, The Lancet, March 15, 2016.
Simon Cauchemez (1), Marianne Besnard (2), Priscillia Bompard (3), Timothée Dub (4), Prisca Guillemette-Artur (5), Dominique Eyrolle-Guignot (6), Henrik Salje (1,7), Maria D. Van Kerkhove (8), Véronique Abadie (9), Catherine Garel (10), Arnaud Fontanet (4,8,11)*, Henri-Pierre Mallet (3)*
(1) Mathematical Modelling of Infectious Diseases, Institut Pasteur, Paris, France
(2) Neonatal Care Department, French Polynesia Hospital Center, Pirae, Tahiti, French Polynesia
(3) Bureau de Veille Sanitaire, Direction de la Santé, Papeete, Tahiti, French Polynesia
(4) Emerging Diseases Epidemiology Unit, Institut Pasteur, Paris, France
(5) Medical Imaging Department, French Polynesia Hospital Center, Pirae, Tahiti, French Polynesia
(6) Gynecology-Obstetrics Departement, French Polynesia Hospital Center, Pirae, Tahiti, French Polynesia
(7) Johns Hopkins University, Baltimore, USA
(8) Centre for Global Health, Institut Pasteur, Paris, France
(9) General Paediatrics Department, Necker Hospital, Paris, France
(10) Department of Pediatric Radiology, Hôpital d’Enfants Armand-Trousseau, Paris, France
(11) Conservatoire National des Arts et Métiers, Paris, France
* These authors had equal senior author contribution.





