What are the causes?
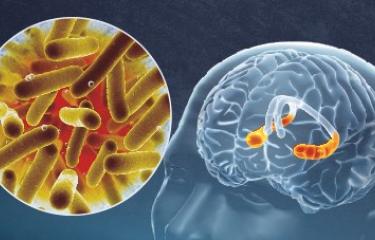
Parkinson's disease is mainly caused by the destruction of dopaminergic neurons in a brain region that controls movement (dopamine is a molecule that controls communication between neurons and is crucial for controlling movement).
It has been proven that the pathological form of a protein in the brain, alpha-synuclein, is capable of triggering neurodegeneration. But the exact causes of Parkinson's disease are not yet known. The scientific community believes that the causes are linked to genetic and environmental factors.
What are the risk factors?
Parkinson's disease is associated with several risk factors. Age is the main risk factor, with an epidemiological peak occurring around the age of 70. Genetics is another factor, but is rarely the sole cause. Finally, the role of exposure to pesticides in the development of the disease has been highlighted.
What are the symptoms?
Diagnosis of Parkinson's disease is based on a number of symptoms:
- intermittent tremors at rest ("resting tremor"), mainly affecting the arms and hands and experienced by around 70% of patients;
- akinesia, i.e. slow execution and coordination of movements, mainly affecting the ability to walk;
- hypertonia, muscle rigidity that is often responsible for a stooped or hunched posture.
Other symptoms are caused by the impact of the disease on the rest of the brain: pain, depression, gut disorders, difficulty sleeping, loss or reduction of smell, balance problems, etc.
Parkinson's is a slow, progressive disease. The first symptoms occur when approximately half of the dopaminergic neurons have been destroyed.
During this initial preclinical phase, which can last for 5 to 10 years prior to symptom onset, the brain uses its plasticity to compensate, and various prodromes, including increased susceptibility to fatigue and concentration problems, may be observed.
The disease progresses through several stages as it becomes more severe, from an initial phase in which clinical signs have no impact on everyday life (Stage 1) to a final phase in which patients lose their autonomy and are unable to walk (Stage 5).
How is Parkinson's disease diagnosed?
Parkinson's disease is mainly based on the patient's medical history and a neurological examination. Medical imaging via an MRI or DaT scan is sometimes used as an additional diagnostic measure to rule out other diseases.
What treatments are available?
There is currently no cure for Parkinson's disease, but there are treatments to help manage symptoms. These include drugs to increase or replace dopamine or to inhibit the enzymes responsible for dopamine degeneration.
But these treatments are purely symptomatic and do not stop disease progression, so they have to be adapted over time if they are to continue being effective. They also do nothing to improve non-motor symptoms, which generally have other causes.
Several years after the emergence of symptoms, the effectiveness of treatments starts to fluctuate and a number of side effects can appear. In these cases, other treatments can be considered: a pump for continuous dopamine delivery to the body, or deep brain stimulation using electrodes.
Various non-drug treatments may also improve the everyday lives of patients. Physical therapy can help address walking and balance issues, while swallowing, speech and writing problems can be resolved through speech therapy.
How can Parkinson's disease be prevented?
There are currently no preventive measures to protect against Parkinson's disease because the exact causes are not known. But maintaining a healthy lifestyle can help reduce the risks.
How many people are affected?
In France, Parkinson's disease is the second most common neurodegenerative disease after Alzheimer's disease and the second leading cause of motor disability in adults after stroke.
Although Parkinson’s disease generally affects older people, 17% of patients are aged under 50, and as the median diagnosis age is 58, many people of working age live with Parkinson's.
September 2024