Salmonella outbreak: Institut Pasteur raises the alarm
The French National Reference Center (CNR) for Salmonella, based at the Institut Pasteur in Paris, is in charge of microbiological surveillance of cases of human Salmonella infection. In late November 2017, it was this CNR that alerted the authorities to the excessive number of salmonellosis cases in infants, prompting action to tackle the outbreak of Salmonella infections linked to powdered baby milk – a story that has hit the headlines in recent weeks. Tasked with monitoring developments and raising the alarm, the CNR plays a vital role in France's wider system for the surveillance and prevention of these infections.
"Between August and December 2017, several infants were identified by the National Reference Center [CNR] for Salmonella as being infected with Salmonella serotype Agona," we read on the website of the French National Public Health Agency (Santé publique France). The identification of eight cases in just eight days by the Institut Pasteur-based CNR in Paris enabled Santé publique France to launch "epidemiological investigations with the parents of the infected infants starting December 1."
The Salmonella CNR (page in French) is a sentinel surveillance system tasked by the French Health Ministry to perform microbiological monitoring of Salmonella outbreaks in France: "We are sent Salmonella strains isolated from patients by private or public laboratories in the CNR's network so that we can carry out highly discriminatory typing and detect any abnormal increases in a particular type," explains Dr. François-Xavier Weill, Director of the CNR at the Institut Pasteur in Paris. The CNR receives nearly 10,000 strains of Salmonella every year, including around 400-600 from babies under the age of one. "Over the past four years [editor’s note: between 2012 and 2016], we have identified around 60 strains of Salmonella Agona each year in patients of all ages," explains Simon Le Hello, Deputy Director of the CNR. François-Xavier Weill points out that, in total, we know of "more than 2,600 different types of Salmonella," and that this Institut Pasteur laboratory is also where Salmonella types are validated at international level.
What should I do with baby milk that I think might be infected?
- Bring it back to the seller in order for the container to be incinerated.
- Wash your hands thoroughly if you have been in contact with milk powder that you think may be infected.
Advice on making up baby formula
- Always wash your hands carefully before and after making up a bottle.
- Once the bottle has been made up, it should be given to the baby straight away or kept in the refrigerator. The bottle should be thoroughly washed as soon as it is finished.

Complete sequencing of bacterial DNA to identify the strain
"For the past year and a half, we have been in a position to perform rapid complete sequencing of the strains we receive for analysis," continues Simon Le Hello. "We have therefore been able to provide microbiological confirmation that the same strain was responsible for infections in several infants under the age of one."
The Institut Pasteur began developing its expertise in the area of Salmonella 70 years ago with the Salmonella Center. In 1972, when the first CNRs were set up in France (see inset below), the center became the Salmonella CNR. This growing expertise on Salmonella was shared and passed on between scientists at the CNR over time. A first outbreak caused by powdered milk contaminated with Salmonella Agona was reported in France in 2005. "Back then it was again our CNR that identified the outbreak, which resulted in almost 140 cases," recalls François-Xavier Weill. The Institut Pasteur keeps all analyzed strains and has an impressive collection of hundreds of thousands of Salmonella strains, some dating back to the end of the 19th century.

The Salmonella CNR at the Institut Pasteur
From 1947 to 1971, the Enterobacteriaceae laboratory directed by Léon Le Minor at the Institut Pasteur served as a reference laboratory for Salmonella. "This scientist asked public and private medical laboratories to send him their Salmonella strains so that he could analyze them in more detail," explains François-Xavier Weill. This strategy gave the laboratory a broad overview of Salmonella cases in France. When the French government officially set up National Reference Centers in 1972, the Institut Pasteur continued to perform this role.
Go to the web page for the Escherichia coli, Shigella and Salmonella CNR (page in french)
Using new techniques that have been available at the Institut Pasteur since 2016 – the PIBnet-P2M platform for complete DNA sequencing and a series of bioinformatics tools developed by the CNR to analyze results –, the scientists recently sequenced the 2005 strain to see how similar it is to the current outbreak. "The current strain is the same as the 2005 strain," confirms Simon Le Hello.
The scientists are continuing to perform retrospective sequencing on collection strains to confirm or disprove the possibility of sporadic cases caused by the same strain occurring between the two outbreaks in 2005 and 2017. This information will be useful for the ongoing inquiry led by French authorities to identify where, when and how the baby milk was contaminated.


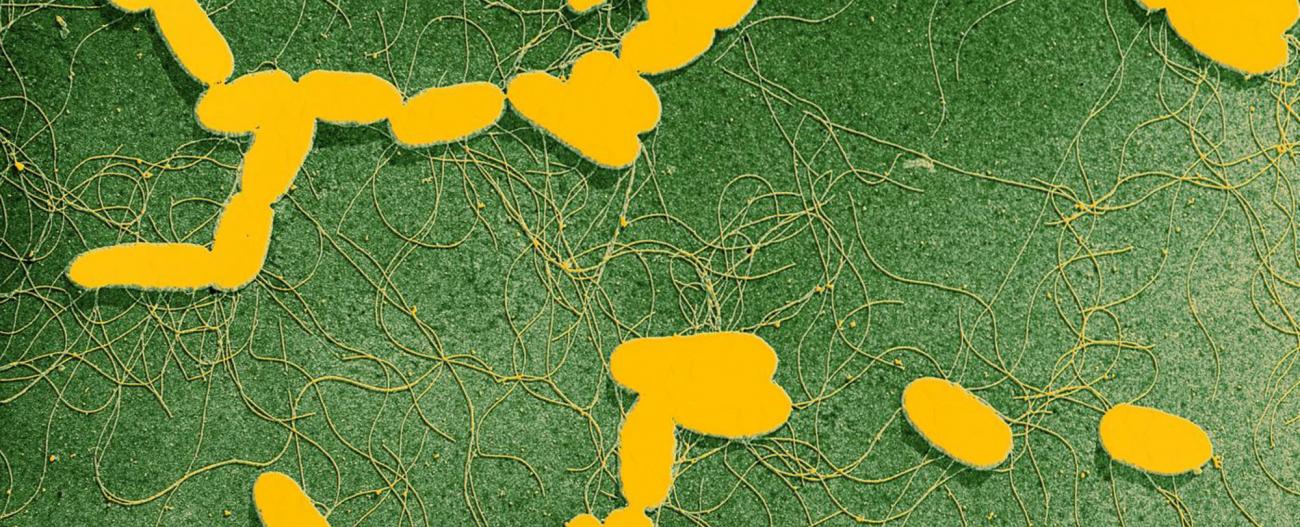
Salmonella in scanning microscopy. © Institut Pasteur
The current strain is the same as the 2005 strain
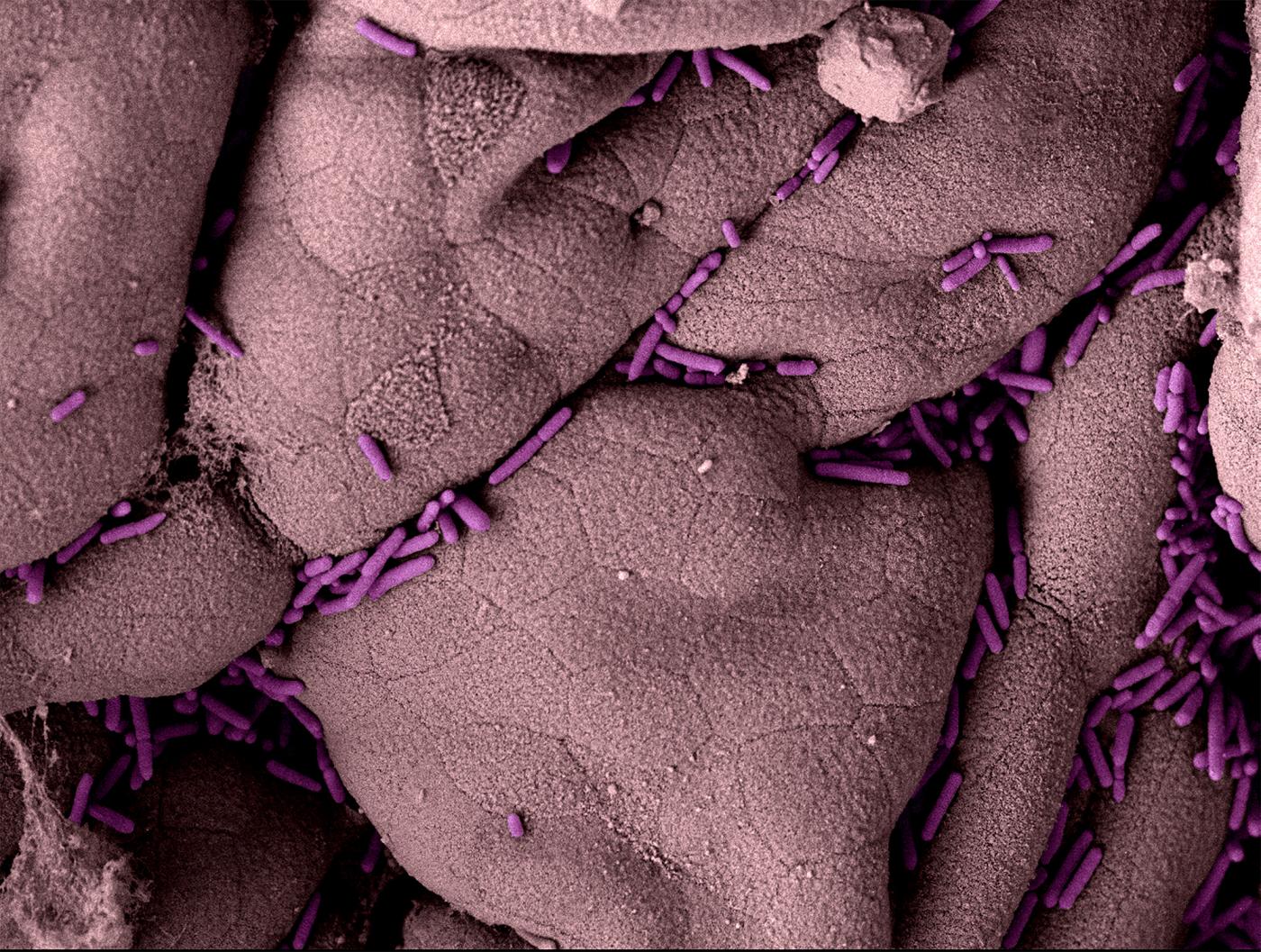
Scanning electron microscopy imaging of interaction between the Salmonella typhimurium bacterium (a different variety from that found during the 2005 and 2017 outbreaks) and the mouse intestinal epithelium. This gram-negative bacillus is responsible for several types of enteritis.
© Institut Pasteur/Perrine Bomme, Ultrastructural Microscopy Platform, Nouara Lhocine, Molecular Microbial Pathogenesis Unit – Image colored by Jean-Marc Panaud.
A safety net
The CNR's role is to fight against communicable diseases – in this case Salmonella. It was given this mission by the French government, which renews its term every five years (the current term runs until 2022). More specifically, the CNR is responsible for microbiological surveillance of cases of human Salmonella infection in communities and hospitals, identifying bacterial strains based on comprehensive epidemiological information.
Go to the web page for the Escherichia coli, Shigella and Salmonella CNR (page in french)
"Our main goal is to identify an outbreak as soon as it begins (a cluster of cases caused by the same type of bacterium over a short period of time). We then raise the alarm and epidemiologists take over to identify where the outbreak began, so that the authorities can issue a recall of the contaminated food," explains François-Xavier Weill. Almost 7,000 isolated strains from human cases are now sequenced every year, most linked to sporadic cases of Salmonella infection. This monitoring of human cases, jointly funded by the French Health Ministry and the Institut Pasteur, is an additional safety net that complements the "farm-to-table" health inspections carried out by the Ministry of Agriculture. "This surveillance system successfully detected both epidemics. It is important to remember this and to reassure any readers who may be worried by what they are seeing in the news," says Simon Le Hello. The recent development of sequencing technologies has revolutionized the microbiological surveillance of these foodborne infections. It is now possible to monitor the development of a given bacterial strain over time. The more surveillance is carried out on a large number of strains, the more effective it is in detecting outbreaks. "Our limits are no longer technological but financial," concludes François-Xavier Weill.


François-Xavier Weill, Director of the National Reference Center for Salmonella at the Institut Pasteur in Paris.
Our limits are no longer technological but financial [to carry out surveillance on increasing numbers of strains].
The role of CNRs in public health surveillance in France
Since the 1950s, France has coordinated efforts to monitor public health, especially in the area of infectious diseases, through National Reference Centers or CNRs (their official name since 1972). The country's CNRs currently operate under the aegis of Santé publique France (formed from the merger between the French Institute for Public Health Surveillance, or InVS, and two other public health organizations). Of the 44 CNRs operating in France in 2017, 14 are hosted by the Institut Pasteur. There are also four CNR-associated laboratories based at the Institut Pasteur in French Guiana.
The centers serve as infectious disease observatories – their mission is to identify or confirm the culprit in suspected cases of infection. To do this they work closely with networks of physicians and laboratories, which directly alert them when new cases occur.
Each CNR focuses its expertise on one specific type of infectious agent. In practice, this surveillance is performed by the heads of research units. CNRs precisely identify which pathogenic strains are in circulation and report any unusual events to the health authorities. These may include the emergence of a new bacterial strain or a cluster of cases that might develop into a more widespread epidemic.
CNRs also provide training for decision-makers and other public health workers.
Learn more about CNRs based at the Institut Pasteur (page in french)
Salmonella and foodborne outbreaks
In Europe, Salmonella is the most frequent cause of foodborne outbreaks and the second leading cause of foodborne disease. Salmonellosis is the name given to infection caused by these intestinal bacteria, which are usually passed on to humans through contaminated food. In human pathology, Salmonella is responsible for two main types of disease: gastroenteritis and typhoid or paratyphoid fever.

"Salmonella" fact sheet


