National Reference Centres, sentinels guarding against pathogens

On December 31, 2022, Santé publique France renewed its trust in the Institut Pasteur for its National Reference Centers (CNRs). Nineteen laboratories are currently involved in the CNRs. Their role is to monitor and analyze circulating pathogens, advance research and protect public health.
Foreword - Being a National Reference Center (CNR)
Definition - What is a sentinel?
Key points - CNRs, sentinels against the unseen
Description - Missions, operation and remit of the CNR
International - Other public health sentinels
Focus - CNRs at the Institut Pasteur
Investigation - Arboviruses: an example of cross-disciplinary surveillance
Key figures - Arboviruses in figures
Chronology - E. coli, Listeria, Salmonella... Anatomy of an alert
Focus - Tracking rabies in real time
Being a National Reference Center (CNR)
With Muhamed-Kheir Taha, Head of the Invasive Bacterial infections Unit and the National Reference Center (CNR) for Meningococci and Haemophilus Influenzae, a designated WHO Collaborating Center for bacterial meningitis
While National Reference Center (CNR) status can only be acquired once scientific expertise has been proven in a specific field, it is nevertheless clear that this expertise develops through "real world" contact with the pathogens targeted by CNRs.
Through its research on the biology of living organisms, the Institut Pasteur works with known microorganisms, which provide genuine test tube models. Alongside the research units, the CNRs monitor and analyze circulating pathogens on a daily basis. This work tests our hard-won knowledge, significantly increasing its reliability and validity by confronting it with an enormously diverse range of pathogen-patient pairings.
The CNRs derive crucial knowledge from this mutual enrichment between basic research and public health. As such, the Institut Pasteur's involvement in 19 of around 40 CNRs operating in France is an undeniable strength, enabling it to advance research and protect public health. CNRs play a key role in health crises. This role as sentinels reflects a specific view of our value.
From its inception, the Institut Pasteur played a major role in public health as a dispensary for rabies treatment as well as a research center for infectious diseases. This role now finds its direct expression in the CNRs' activities. They reflect recognition of our scientific expertise and ability to collaborate within the epidemiological surveillance ecosystem. In recent years, the CNRs have become bona fide decision-making tools for the public authorities, extending their role as sentinels to become key stakeholders in a coordinated response to pathogenic threats.
As recognized by the scientific community and public, the CNRs continue to prove their worth by responding early to emerging health crises and helping to prevent many others. We can only be proud of contributing to their success and thus continuing to pursue the Institut Pasteur's original mission.
What is a sentinel?
With Isabelle Cailleau, Institut Pasteur Medical Department, coordinator of the National Reference Centers
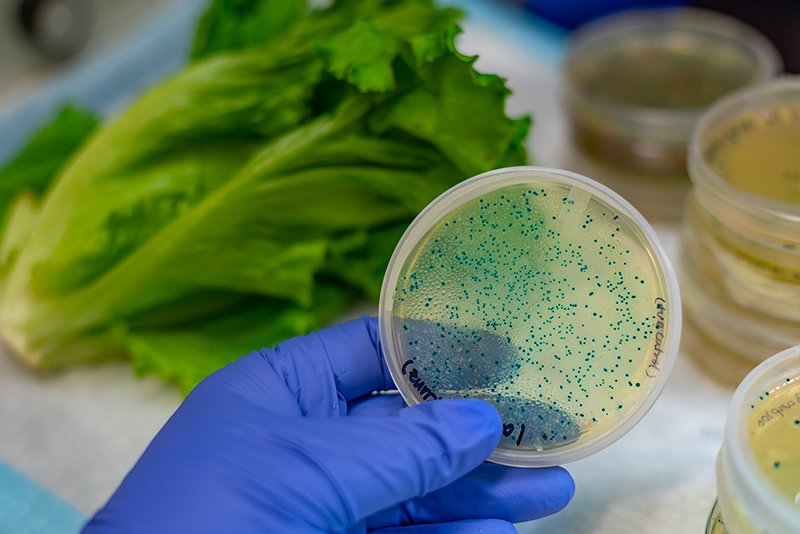
E. coli contamination in romaine lettuce. Credit: Adobe Stock
sentinel, noun:
something that guards, protects, keeps watch; whose task is to provide surveillance and thus prevent any surprises. With its origins in military terminology, the term "sentinel" conjures images of an outpost or strategic position enabling the detection of changes or anomalies indicative of things to come. The sentinel stands guard, a beacon in the mist of a potentially hostile "other" against which protection is sought.
In public health terms, the word "sentinel" refers to a surveillance process. National Reference Centers (CNRs) are watchtowers that gather, analyze and interpret signals of potential future outbreaks.
CNRs offer specific expertise in terms of identification, characterization and vigilance. They are required to analyze, contextualize and interpret large volumes of data and link them to existing scientific knowledge. The alert mechanism is therefore just a first step, triggering a process that is honed to ensure an immediate and effective response.
A CNR is an interface. It is a place in which knowledge of microorganisms and their hosts gained through basic research is confronted with pathogen strains sent by medical test laboratories as part of epidemiological surveillance. A place where the controlled laboratory environment meets unpredictable crisis situations. Each side benefits from the other in a cycle enabling the continual improvement of knowledge of diseases, their vectors and modes of transmission. Expertise and models are compared, bounced off each other, shaken up and refined by sentinels, which represent a strength and asset, not just for public health but also research.
CNRs, sentinels against the unseen
With Isabelle Cailleau, Institut Pasteur Medical Department, coordinator of the National Reference Centers

Manipulation at the CNR of rabies - Lyssavirus epidemiology and neuropathology. Copyright: William Beaucardet.
National Reference Centers (CNRs) are early warning stations for outbreaks, sweeping French national territory in their role as look-outs for threats with potential public health implications. Supported by research units, they draw on the expertise of leading scientists and access state-of-the-art technologies. All this enables them to constantly update existing knowledge of the virulence and transmission mechanisms of infectious agents and methods of detecting them. Their value to the health ecosystem and our ability to understand, anticipate and respond to unseen threats has been clearly demonstrated by the key role they have played in managing recent health crises.
A long-standing surveillance system
The designation "National Reference Center" (CNR) made its first appearance in France in an order published in the Official Journal of April 18, 1972. However, the notion of "reference centers" had already been used since the 1950s to describe the activities of Institut Pasteur research units in response to issues raised by physicians or the French Ministry of Health regarding the diagnosis or treatment of certain infectious diseases.
Going back even further, the Institut Pasteur has, since its very early days, naturally assumed a role as sentinel for numerous communicable diseases. Its original articles of association provided for: "creation and management of laboratories for referral, testing and monitoring, and for collections of microbial strains", which fully encapsulates the CNR concept.
Obviously, the system has since been developed to keep pace with the speed and scale of these pathogenic threats and harness progress in detection techniques. Official recognition of CNRs in 1972 brought confirmation of their role as sentinels and harmonization of their remit at national level. There are currently 43 of them following the renewal of their term of office in early 2023. Thirteen of these are coordinated by the Institut Pasteur (see list on page 14), each specializing in a pathogen or pathogen family.

Prof. Christophe Burucoa
Chairman of the CNR Committee,
Santé publique France
"The CNRs play a central role in our public health system, working closely with Santé publique France. They provide essential microbiological support to strengthen our ability to respond to developments in pathogen spread. Besides acting as sentinels, they are also interfaces between research and public health and forums for vital discussions between all stakeholders, both at local and national level."
An extended remit in the post-pandemic landscape
The CNRs' response to recent health crises (see timeline further on) has confirmed their key role in the outbreak alert and response process. Their ability to combine basic research, expertise gained in medical biology through the CNR remit, and scientific breakthroughs in predictive epidemiology makes them the first link in the chain of a coordinated response. The SARS-CoV-2 outbreak perfectly illustrates the value of concurrent interactions between research and its applications, including large-scale, real-time data collection and analysis to track the development of the outbreak, the introduction of screening tests, and support for national health agencies with assessments of diagnostic tests, all of which proved the CNRs' key role in managing this most recent health crisis.
The call for applications to renew CNRs published in March 2022 extended the remit (see diagram) of some CNRs including the Center for Respiratory Infection Viruses, which was tasked with developing a range of techniques and methods to enhance its expertise on coronaviruses and respiratory syncytial virus responsible for respiratory infections such as bronchiolitis, very severe forms of which can occur in infants.
Research and public health: sharing best processes
Having long been confined to their role as observatories for pathogens, CNRs have gradually been upgraded as key interfaces between basic research and public health. By logging and analyzing thousands of pathogen strains every year, CNRs accumulate substantial, constantly updated collections that can be used to track the spread of a disease over time and characterize successive mutations of a microorganism, thus providing a valuable record of diseases and outbreak development. This, for instance, enabled teams from the CNR for Vibrios and Cholera to investigate the genomes of 172 strains in 2020 to elucidate the source of cholera outbreaks since 1970 and confirm the role of humans in their spread. These databases form the bedrock of epidemiological surveillance, and analysis of them supports modeling work used to forecast the development of outbreaks and guide health authorities on introducing protective measures to limit their spread. Moreover, samples collected by CNRs provide research units with valuable material with which to conduct their basic research and studies. Scientific papers and discoveries at the Institut Pasteur are furthermore increasingly based on data collected by CNRs.
CNRs' affiliated laboratories also offer expertise that brings significant public health benefits, particularly with regard to technical progress. In one recent example, the source of a salmonella contamination of powdered milk that infected nearly 200 infants between 2005 and 2017 (for which an alert was issued by the CNR for Escherichia coli, Shigella and Salmonella) was identified thanks to progress on high-throughput genome sequencing, a technique used in the Institut Pasteur's Enteric Bacterial Pathogens Unit.
Missions, operation and remit of the CNR
The CNRs' missions
- concerning the microbiology and pathology of infectious agents, the development, optimization, validation and distribution of medical biology examinations; the identification and confirmation of pathogens;
- Scientific or technical advice in response to any request from the French Health Minister, Santé publique France (SpF) and health professionals;
- The contribution to epidemiological surveillance:
-by leading a network of laboratories responsible for handling examinations and subsequently transmitting results,
- by carrying out the analyses necessary for the monitoring of pathogens
- Immediately alerting Santé publique France, the French Ministry of Health, and, where applicable, the Regional Health Agency to any finding likely to present a risk or threat to public health.
Operation and remit
CNRs are appointed for a five-year period by the French Ministry of Health on the basis of proposals from Santé publique France following an assessment of applications by a committee of experts. Specifications are drawn up setting out specific missions for each CNR. To conduct certain missions, a CNR can rely on one or more laboratories (no more than three) known as "associated laboratories." To ensure their missions are performed optimally, CNRs are involved in numerous national and international collaborations, particularly with public and private medical test laboratories, physicians from the "Sentinelles" network, Santé publique France for epidemiological surveys, health authority departments, research laboratories and organizations (Inserm, CNRS, Anses, Ifremer, etc.) and industrial laboratories. Most CNRs are also members of European networks (including the European Centre for Disease Prevention and Control – ECDC) or international networks (the World Health Organization (WHO) – see below).
Other public health sentinels
Like pathogens themselves, surveillance systems are unconfined by geographic borders! International health institutions throughout the world have formed sentinel networks composed of reference laboratories.
World Health Organization (WHO) Collaborating Centers coordinate international efforts under the aegis of the organization. The Institut Pasteur hosts seven of these centers in France (Enterovirus, Listeriosis, Meningitis, Rabies, Salmonella, Antimalarial Drug Resistance and Yersinia), while Pasteur Network members host 17 worldwide.
The WOAH (World Organization for Animal Health) operates by the same principle of a network of collaborating centers. The Institut Pasteur hosts the center for the detection and identification in humans of emerging animal pathogens and development of tools for their diagnoses.
Finally, the Institut Pasteur set up a Laboratory for Urgent Response to Biological Threats (CIBU) in 2002 at the instigation of the French General Directorate of Health. With its 24/7 on-call system, the team can respond to microbiological emergencies both in France and worldwide at the request of the French General Directorate of Health. It supports the CNRs as seen in the early days of the COVID-19 pandemic and the H1N1 influenza pandemic in 2009. The CIBU is a World Health Organization partner whose remit also includes tackling emerging diseases such as Ebola in Guinea and the Democratic Republic of the Congo.
CNRs at the Institut Pasteur
The Institut Pasteur hosts 19 laboratories (13 coordinating and 6 associated laboratories). These monitor the following 17 pathogens:
Viruses
- Respiratory infection viruses including influenza and SARS-CoV-2
- Rabies virus
- Viruses causing hemorrhagic fevers such as Lassa and Ebola
- Hantaviruses spread by rodents
- Arboviruses (see article at the end of this special feature)
- Enteroviruses and parechoviruses, particularly those causing poliomyelitis
Bacteria
- The genus Clostridium including the bacterium causing botulism
- The genus Yersinia including the plague bacillus
- The genus Corynebacterium including the bacterium causing diphtheria
- The genera Shigella, Salmonella and Escherichia coli responsible for foodborne infections
- The genus Leptospira that can cause kidney failure
- The genus Listeria including "refrigerator bacteria" that cause listeriosis
- Meningococci and Haemophilus influenzae, which cause meningitis
- Vibrios including the cholera agent
- The genus Bordetella including the whooping cough bacillus
Fungi
- Candida, aspergillus, cryptococcus and other invasive mycoses
Parasites
Arboviruses: an example of cross-disciplinary surveillance
Dengue, chikungunya, yellow fever and Zika are severe diseases caused by the same virus type: "arboviruses". These viruses spread to vertebrates through bites from blood-feeding vectors (insects or ticks). Carriers include mosquitoes mainly from the genus Aedes, such as Aedes albopictus (the tiger mosquito) and Aedes aegypti. Their eggs are able to survive for several months in dry environments and, in the case of the tiger mosquito, even in cold environments. They are identified as invasive species.

Origins and emergence
The Zika virus was first detected in a monkey in Uganda in 1947. The first outbreak hit Micronesia in 2007 and was followed by further outbreaks in French Polynesia in 2013 and 2014, and Brazil in 2015.
Dengue is most prevalent in intertropical regions. Cases have been regularly reported in France since 2010, proving that transmission is a genuine risk, even in temperate zones.
Yellow fever was rife in the Americas between the 17th and 19th centuries. It is now most prevalent in Africa, with 95% of cases reported in this continent.
Since the first chikungunya outbreak in Tanzania in 1952, the disease has gained ground in Africa and Asia. The virus emerged in Europe in 2007, subsequently spreading to the West Indies and Polynesia, with major outbreaks between 2013 and 2014.
Transmission
A bite by a mosquito of the genus Aedes, the virus vector. A single mosquito can carry nearly 10 billion viral particles without suffering any harmful effects itself. Once infected, the mosquito can transmit the virus throughout its lifespan with every bite.
Expertise and surveillance
Almost 60% of the units in the Institut Pasteur Department of Virology in Paris work on vector-borne diseases.
The Laboratory for Urgent Response to Biological Threats (CIBU) is part of the WHO Collaborating Center for Arbovirus and Viral Hemorrhagic Fever Reference and Research. It is particularly involved in diagnosing and researching Zika virus.
The Institut Pasteur de la Guyane hosts the associated laboratory for the National Reference Center for Arboviruses.
A medical entomology course has run since 1988, providing training in this discipline to experts from around the world. The course runs every two years, alternating with a course via the Pasteur Network. A MOOC version is also available.
The Institut Pasteur and other Pasteur Network members are part of the Arbo-france French multidisciplinary and multi-institutional monitoring, surveillance and research network on human and animal arboviruses (arbo-france.fr).
Arboviruses in figures
100M
symptomatic cases of dengue
per year worldwide, including 500,000
hemorrhagic cases (source: WHO)
200,000
cases of yellow fever per year wordlwide
with mortality rates ranging from
20 to 60% depending on the outbreak
(source: WHO)
1 chikungunya vaccine candidate
produced by the Viral Genomics
and Vaccination Unit, which is
ready to enter Phase III
Anatomy of an alert
With François-Xavier Weill, Director of the CNR for Escherichia coli, Shigella and Salmonella
Prologue
CNRs play a pivotal role in a well-established system governing the surveillance of pathogens. What is the process for switching from sentinel to alert status? Here is a close look at one potential scenario…
Step 1: the threat
Cases of infection with a pathogen that is under surveillance are reported in various parts of the country. These have been identified by both hospital-based and non-hospital-based medical test laboratories that have diagnosed one or more patients. Two scenarios:
- either the disease in question is designated as notifiable (there were 36 such diseases in 2022), in which case any samples taken from patients are sent to the dedicated CNR for analysis of the responsible strains;
- or it is not designated as a notifiable disease but strains are submitted for microbiological surveillance and may be sent to the CNR for characterization and typing to identify the source of an infection or detect a chain of infection.
Step 2: expert assessment
Any samples received are identified using advanced technologies (genome sequencing since 2017) to precisely type the exact strain of the responsible pathogen. This microbiological work involves comparing the sampled pathogen with a genome database to determine other genetically related strains and thus trace the outbreak's origins. The results of these analyses are then passed on to Santé publique France, so it can assess the epidemiological situation. This is done in real time for notifiable diseases and at regular intervals for other diseases. For foodborne infections, any samples taken from potentially contaminated food or subject to systematic surveillance are passed on to the CNR for comparison of strains taken from clinical samples with strains taken from food samples in an attempt to identify the source of contamination.
Step 3: the alert
In most cases, the identified pathogen is known. Sometimes, a new strain or variant is identified, adding to knowledge of the associated disease. An alert is issued once the situation exceeds known parameters for normal circulation. This occurs in cases where a new, more aggressive and/or more communicable and/or more antibiotic-resistant strain is identified. Sometimes, case numbers rise quickly or their geographic concentration suggests a common source of infection. All situations are closely monitored to prevent a potential outbreak. The CNR teams immediately alert Santé publique France, which may decide to expedite an epidemiological survey to ascertain the source of contamination. Other institutional stakeholders may also become involved depending on the pathogen type. These include the general directorates of ministries (of agriculture/food, health, the economy, etc.) if the investigation relates to a foodborne infection.
Step 4: monitoring and advice
Once the alert has been issued, the CNRs continue their work in two parallel areas. The first involves monitoring the development of the emergence with enhanced case tracking to map the circulation of the responsible strain. The second involves supporting the public health authorities with insights on how to respond to the alert, for example by recommending the most appropriate diagnostic testing methods for the identified strain.
Epilogue
The outbreak has been contained, its source identified, and measures taken to prevent its resurgence. However, the CNR's role as a sentinel does not stop there. It continues to monitor circulating pathogens and keeps records of this latest alert, which constitute a vital tool for quickly identifying any future re-emergences of infection. Some CNRs store all the strains they receive over periods spanning decades (for example, the CNR for Escherichia coli, Shigella and Salmonella has retained hundreds of thousands of strains since 1947). This valuable knowledge supports the work of research units, shedding light on pathogens' genetic diversity and evolution over time. Some CNRs also conduct cohort tracking surveys, which involve monitoring a defined population over time to study the incidence of health events in order to improve our understanding of diseases.
Tracking rabies in real time
Rabies is the type of pathogen we like to monitor closely. Every year, the CNR for Rabies (CNRR) analyzes between 1,200 and 1,300 samples from animals as part of its surveillance work. In October 2022, an alert was triggered by a case of canine rabies in the Greater Paris Region. Here is an hour-by-hour summary.
with Laurent Dacheux, Deputy Director of the CNR for Rabies.