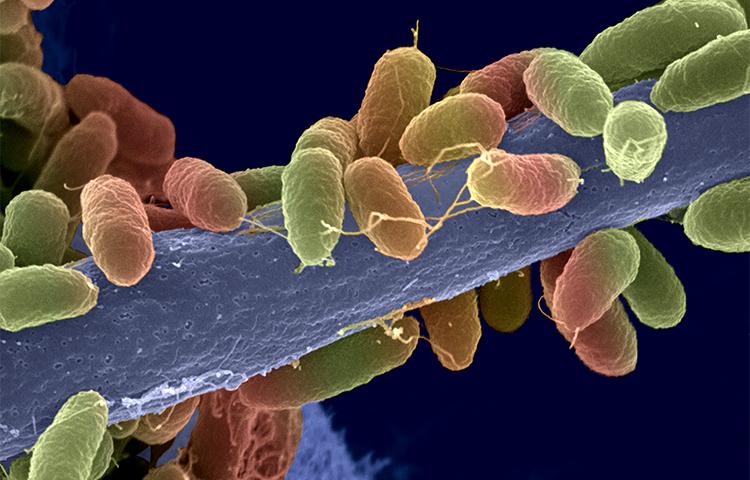
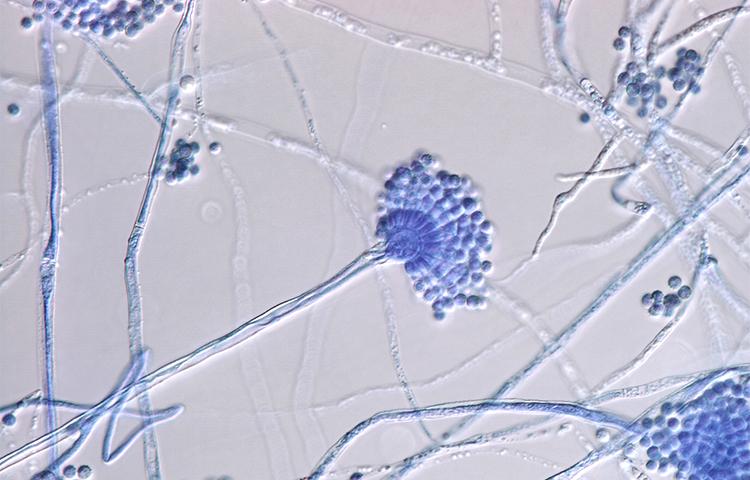
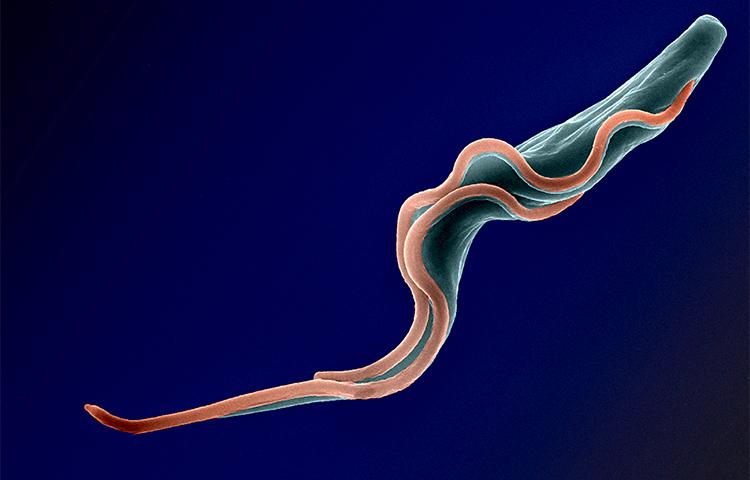
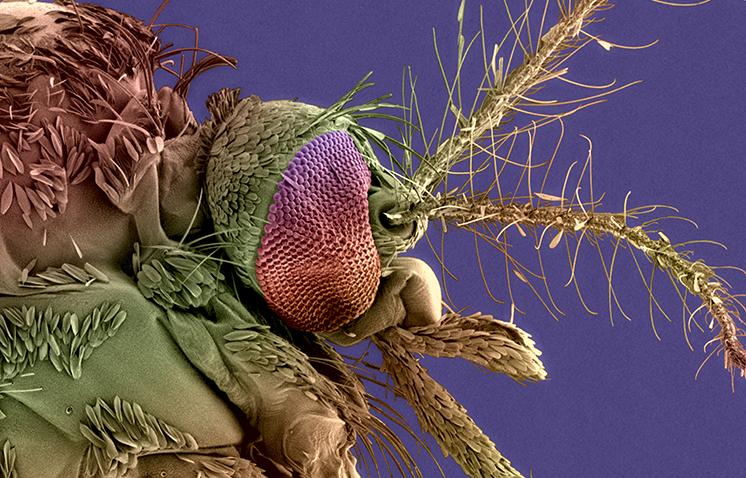
The global rise in antimicrobial resistance means that we are at risk of heading towards a post-antibiotic era, where common infections once again become life threatening. This dire prediction has raised awareness at the highest levels, including the United Nations and the G20. Therapy escape and the need for more effective treatments are not restricted to bacteria; they concern all microorganisms (viruses, fungi and parasites) and their vectors. Challenges include the emergence of resistance of the malaria parasite Plasmodium falciparum to artemisinin, the most effective treatment, and mosquitoes’ ability to change their behavior to counter insecticides.
AIMS
- To improve understanding of resistance emergence and dissemination by combining approaches involving epidemiology, genomics, statistics, evolutionary biology, structural biology, chemical biology and modeling to identify factors contributing to the spread of resistant strains and resistance genes.
- To analyze the physiology, ecology and evolution of microorganisms and their vectors. The molecular mechanisms governing microbial growth, metabolism and acquisition of resistance will be studied. For example, structural and chemical biology allow to characterize the mode of action of resistance at the molecular level. The complex interactions between the host and communities of microorganisms need to be taken into account to understand resistance. We aim at analyzing the formation of complex structures (e.g. biofilms) and the processes of quiescence, dormancy, persistence and tolerance, which represent additional means of treatment escape.
- To identify new drugs and therapeutic strategies in response to antimicrobial resistance. We are synthetizing focused chemical libraries and exploring new targets, as those involved in host-microbe interaction and in the life cycle of the infectious agents. Phenotypic and molecular screening are implemented to identify selective inhibitors, phage therapy is further explored and diverse environments are exploited to find new natural products. In parallel, we aim at novel vaccines and immunotherapies to target microbes and resistant strains.
MEASURES
- Recruit two five-year research groups (G5s)/research units.
- Propose research funding that encourages novel synergistic and interdisciplinary approaches for the development of new treatments and alternative strategies to tackle infections.
- Adopt metabolomics analysis techniques to examine microbes and their hosts.
- Build a collaborative network of clinicians and public health experts.
- Involve research units in the International Network in research on resistance.
- Foster public-private partnerships for diagnostics and antimicrobial drug development.
PRINCIPAL COORDINATORS:
Philippe Glaser, Head of Ecology And Evolution of Antibiotics Resistance Unit
Paola B. Arimondo, Head of Epigenetic Chemical Biology Unit
CONFERENCE 2020
Joint Conference on Antimicrobial Drug Development
17 April 2020 at Institut Pasteur
Amphithéâtre Duclaux, 28 rue du Docteur Roux, 75015 Paris, France
Organized by
International Research Alliance for Antibiotic Discovery and Development (IRAADD)
German Center for Infection Research (DZIF)
Institut Pasteur (axe 2- AMR)
DEDICATED TEAMS
EVENTS
First Workshop of the strategic focus 2 “AntiMicrobial Resistance - AMR” 7th October 2019
Scientific board:
- Didier Ménard
- Lulla Opatovski
- Thierry Fontaine
- Didier Mazel
- Anna Bella Failloux
- Felix Rey
- Fabrice Agou
- Kathleen Victoir