In collaboration with the universities of Miami, Columbia and San Francisco, scientists from the Institut Pasteur, Inserm, CNRS, Collège de France, Sorbonne University and the University of Clermont Auvergne have managed to restore hearing in an adult mouse model of DFNB9 deafness – a hearing disorder that represents one of the most frequent cases of congenital genetic deafness. Individuals with DFNB9 deafness are profoundly deaf as they are deficient in the gene coding for otoferlin, a protein which is essential for transmitting sound information at the auditory sensory cell synapses. By carrying out an intracochlear injection of this gene in an adult DFNB9 mouse model, the scientists successfully restored auditory synapse function and hearing thresholds to a near-normal level. These findings, published in the journal PNAS, open up new avenues for future gene therapy trials in patients with DFNB9.
Over half of nonsyndromic profound congenital deafness cases have a genetic cause, and most (~80%) of these cases are due to autosomal recessive forms of deafness (DFNB). Cochlear implants are currently the only option for recovering hearing in these patients.
Adeno-associated viruses (AAVs) are among the most promising vectors for therapeutic gene transfer to treat human diseases. AAV-based gene therapy is a promising therapeutic option for treating deafness but its application is limited by a potentially narrow therapeutic window. In humans, inner ear development is completed in utero and hearing becomes possible at approximately 20 weeks of gestation. In addition, genetic forms of congenital deafness are generally diagnosed during the neonatal period. Gene therapy approaches in animal models must therefore take this into account, and gene therapy efficacy must be demonstrated following a gene injection when the auditory system is already in place. In other words, therapy must reverse existing deafness. The team led by Saaïd Safieddine, a CNRS researcher in the Genetics and Physiology of Hearing Unit (Institut Pasteur/ Inserm) and coordinator of the project, used a mouse model of DFNB9, a form of human deafness that represents 2 to 8% of all cases of congenital genetic deafness.
DFNB9 deafness is caused by mutations in the gene coding for otoferlin, a protein that plays a key role in transmitting sound information at the inner hair cell synapses. Mutant mice deficient in otoferlin are profoundly deaf as these synapses fail to release neurotransmitters in response to sound stimulation, despite the absence of detectable sensory epithelial defects. DFNB9 mice therefore constitute an appropriate model for testing the efficacy of viral gene therapy when it is administered at a late stage. However, as AAVs have limited DNA packaging capacity (approximately 4.7 kilobase (kb)), it is difficult to use this technique for genes whose coding region (cDNA) exceeds 5 kb, such as the gene coding for otoferlin, which has a 6 kb coding region. The scientists have overcome this limitation by adapting an AAV approach known as dual AAV strategy because it uses two different recombinant vectors, one containing the 5’-end and the other the 3’-end of the otoferlin cDNA.
A single intracochlear injection of the vector pair in adult mutant mice was used to reconstruct the otoferlin coding region by recombining 5' and 3'-end DNA segments, leading to long-term restoration of otoferlin expression in the inner hair cells, and then restored hearing.
The scientists have therefore obtained initial proof of the concept of viral transfer of fragmented cDNA in the cochlea using two vectors, showing that this approach can be used to produce otoferlin and durably correct the profound deafness phenotype in mice.
The outcomes achieved by the scientists suggest that the therapeutic window for local gene transfer in patients with DFNB9 congenital deafness could be wider than thought, and offers hope of extending these findings to other forms of deafness. These results are the subject of a patent application filed.
In addition to the institutions mentioned in the first paragraph, this research was funded by the French Foundation for Medical Research, the European Union (TREAT RUSH) and the French National Research Agency (EargenCure and Lifesenses LabEx).
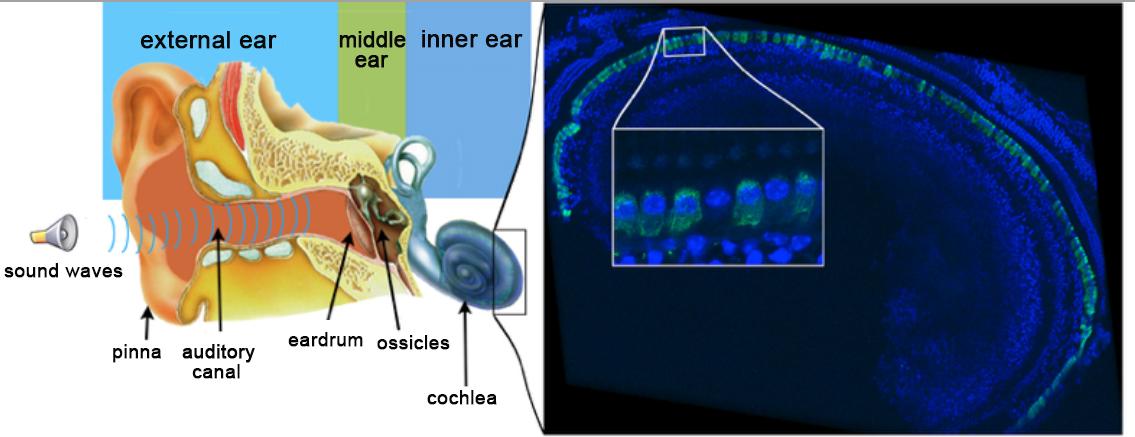
The left panel is a schematic representation of the human ear. Sound waves are collected by the outer ear made up of the pinna and ear canal. The middle ear, composed of the eardrum and ossicles, transmits sound waves to the inner ear, which features the cochlea – the hearing organ responsible for transmitting auditory messages to the central nervous system. The right panel shows an immunofluorescence image of the auditory sensory epithelium within an injected cochlea. The inner hair cells have been stained for otoferlin in green. Otoferlin is detected in almost all of these cells. The inset is a high magnification area showing an inner hair cell that has not been transduced. © Institut Pasteur
[1] Research published by the Institut Pasteur and Inserm Genetics and Physiology of Hearing Unit (UMRS1120): "Otoferlin, defective in DFNB9 deafness, is essential for synaptic vesicle exocytosis at the auditory ribbon synapse" Cell, October 20, 2006
Source
Dual AAV-mediated gene therapy restores hearing in a DFNB9 mouse model, PNAS, February 18, 2019
Omar Akil*§§, Frank Dyka†, Charlotte Calvet‡,§,¶, Alice Emptoz‡,§,¶, Ghizlene Lahlou‡,§,¶, Sylvie Nouaille‡,§,¶, Jacques Boutet de Monvel‡,§,¶, Jean-Pierre Hardelin‡,§,¶, William Hauswirth†, Paul Avan#, Christine Petit‡,§,¶,**,¶¶, Saaid Safieddine‡,§,¶,††,¶¶, Lawrence R. Lustig‡‡,§§
*Department of Otolaryngology-Head & Neck Surgery, University of California San Francisco, San Francisco, CA, USA
†Department of Ophthalmology, University of Florida, College of Medicine, Gainesville, FL, USA
‡Genetics and Physiology of Hearing Laboratory, Institut Pasteur, Paris, France.
§Institut National de la Santé et de la Recherche Médicale (Inserm UMRS 1120), Paris, France
¶Sorbonne Universités, UPMC Université Paris 06, Complexité du Vivant, Paris, France
#Laboratoire de Biophysique Sensorielle, Faculté de Médecine, Université Clermont Auvergne, Biophysique Médicale, Centre Jean Perrin, Clermont-Ferrand, France.
**Collège de France, Paris, France
††Centre National de la Recherche Scientifique, France
‡‡Department of Otolaryngology-Head & Neck Surgery, Columbia University Medical Center, and New York Presbyterian Hospital, USA
§§Joint senior authors
¶¶ Corresponding authors